Diabetic Retinopathy
Diabetic Retinopathy Treatments NYC by Marc Bystock L.Ac.
Call Marc Bystock L.Ac.
"Hi, my name is Marc Bystock. I’m a licensed acupuncturist located in New York City and in practice since 1996.
I specialize in treating patients who have degenerative eye conditions. I use a variety of acupuncture systems to address the needs of my patients, including Micro-acupuncture, Acunova acupuncture, Traditional Chinese Medicine. These acupuncture systems are specific for the treatment of eye disorders. Most patients show signs of positive improvement within the first two weeks of treatment."
-Marc Bystock L.Ac.
Contact Marc Bystock, Leading Holistic Acupuncturist in NYC for a Free Consultation.
CONTACT MARC
VERIFY YOUR HEALTH INSURANCE
Acupuncture for Diabetic Retinopathy by Marc Bystock NYC Acupuncturist in Midtown Manhattan NY 10016
What is Diabetic Retinopathy?
Diabetic retinopathy is a condition of the eyes that may occur when blood glucose-sugar exceeds normal levels over a prolonged period. This may result in a decline in vision and blindness in some cases. Within the aged population of the United States, diabetic retinopathy remains a leading causative factor of blindness.
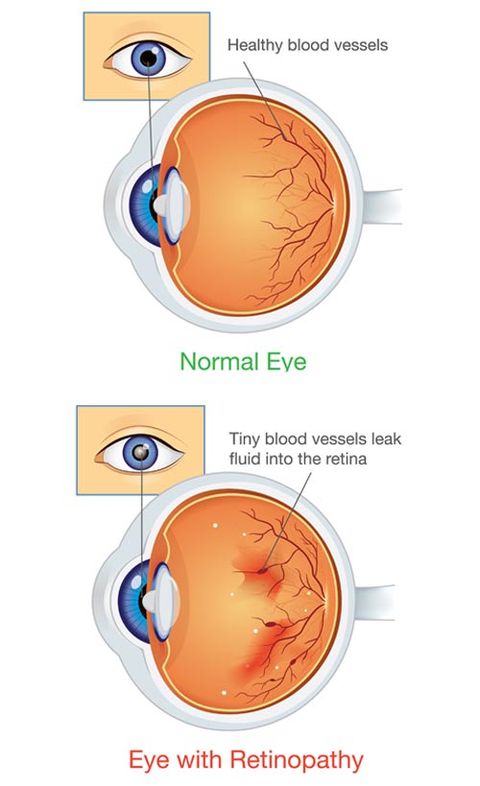
The retina consists of layers of cells located at the back of the eye. These light-sensitive cells convert light to electrical impulses that signal the brain. The brain converts these signals into images of vision. In order for the retina to function correctly, it requires a constant blood supply. Blood is transported through tiny vessels that are very fragile to any adverse conditions.
There are three distinct stages of diabetic retinopathy:
- The earliest stage is called: background retinopathy. In this stage, small bulges can occur in the vessels causing minor bleeding, usually without any vision loss.
- The second stage is called: non-proliferative diabetic retinopathy (NPDR). When the macula swells, macula edema may occur, causing loss of vision.
- The third stage is known as proliferative diabetic retinopathy (PDR). It is characterized as the most advanced stage and signifies neovascularization. This means the growth of new blood vessels. Since these new blood vessels are very fragile, they can easily bleed out into the vitreous. This may also cause vision loss. The transparent gel material supports the eye to maintain its oval shape. Millions of small fibers in the vitreous humor attach to the retina’s cell surface, where light sensitivity is enhanced.
What Causes Diabetic Retinopathy?
Diabetes causes insulin resistance throughout the body, which leads to both physiologic and metabolic changes. High blood sugar levels and insulin resistance cause oxidative stress, inflammation, and insufficient blood perfusion to the optic nerve and the light-sensitive tissue called the retina located in the back of the eye. The tiny blood vessels that innervate the ocular region begin to swell, leaking both fluid and blood.
Scarring can occur from new vessel growth and may lead to damage of the macula or a detached retina. Initially, the diabetic retinopathy patient may feel no symptoms. However, after disease progression, the condition becomes so advanced that vision loss may become noticeable.
What are the Symptoms of Diabetic Retinopathy?
When small blood vessels are inflamed and damaged, they can form clots, close up and develop balloon-like protrusions call microaneurysms. Newly formed blood vessels grow to replace them surrounding the macular, which will block the patient’s vision.
Symptoms may include distorted blurry vision in the early stages and double vision in more advanced cases. MMany diabetic retinopathy patients will experience eye floaters. Floaters are the name for small dark black specks that appear to move in our field of vision.
For many who experience diabetic retinopathy, both night vision and color vision may fluctuate and become problematic. Finally, in later stages of diabetic retinopathy with macular edema and leaking fluid, both pain and vision loss may become problematic symptoms for patients.
How I Use Acupuncture to Treat Diabetic Retinopathy
Traditional Chinese Medicine (TCM) can treat patients with diabetes and diabetic retinopathy. Traditional Chinese Medicine treats at the underlying root level of any disorder. In other words, causative case factors must first be determined; then, functional changes must be made to optimize the body’s function.
Diabetic retinopathy requires simultaneous support of the spleen, pancreas, and the digestive system to manage diabetes as well as direct treatment of the eyes themselves.
The condition of the gastrointestinal tract and the organs involved may be improved by the use of a specific food plan, low in glycemic index and high in nutrient value. In addition, selective herbs and nutrients may reduce inflammation and help return the body to a balanced state.
Acupuncture will be performed to address any bleeding of the micro-circulatory system that feeds the retina and surrounding tissue. By improving blood perfusion to the eyes, oxygen and nutrient delivery are both encouraged. With increased nutrients and blood flow to the eyes, vessels strengthen, fatty deposits are reduced, and macula edema may be resolved.
What is the Conventional Medical Treatment for Diabetic Retinopathy?
Conventional medical wisdom calls for both your family physician and your ophthalmologist to work with you simultaneously. Your regular doctor should help to control your diabetes and lower your blood sugar levels. Your eye specialists can treat your eyes directly using a laser procedure termed a vitrectomy. This detailed surgical process removes the vitreous humor to provide access to the retina for repair and scar tissue extraction.
Contact NYC Acupuncturist Marc Bystock L.Ac. for Diabetic Retinopathy Treatments
I specialize in treating patients who have degenerative eye conditions. I use a variety of acupuncture systems to address the needs of my patients, including Micro-acupuncture, Acunova acupuncture, Traditional Chinese Medicine. These acupuncture systems are specific for the treatment of eye disorders. Very thin acupuncture needles are placed on the hands, the feet, and around the eyebrows (Never in the eyes).
In addition, depending on the disorder being treated, I may use electrical stimulation, cold laser therapy, pulsed electromagnetic frequency therapy, specific food plans, herbs, and nutrients. Most patients show signs of positive improvement within the first two weeks of treatment. Results may vary depending on a variety of circumstances.
If you have diabetic retinopathy with or without any vision loss or you know a friend or family member who has been diagnosed with this degenerative eye disorder, please contact me as soon as possible so that we can discuss a treatment strategy that will work for you. I look forward to helping you!
Please contact me
today!
Additional Links
Treatment Hours
- Monday
- -
- Tuesday
- -
- Wednesday
- -
- Thursday
- -
- Friday
- -
- Saturday
- -
- Sunday
- Closed
Copyright 2019 Marc Bystock All Rights Reserved. Art licensed by Shutterstock